By Mandy Tam, R.Ac · Founder, Artemis Wellness Clinic Richmond BC
Reviewed by: Mandy Tam, R.Ac · Date: [PENDING]
When new patients come in for their first acupuncture session, the question I get asked most often is: “But what IS a meridian, really?” And the honest answer takes longer than thirty seconds, so I want to write it down properly here.
I have been in clinical practice for over a decade. I have treated thousands of people in Richmond and across the Lower Mainland — engineers, nurses, mothers, retirees, skeptics, believers. The skeptics are usually the ones who ask the meridian question first, and I respect that. They want to know what is actually going on in their body when I place a needle, not just hear poetic language about “energy flow.” This article is for them — and for any patient who has ever wondered if there is something real underneath the ancient vocabulary.
What I want to give you here is not a sales pitch for acupuncture. It is the honest, working understanding I have built up over ten years of seeing what helps people and what does not. Some of it is rooted in classical Chinese medical theory. Some of it overlaps with what modern fascia and neuroscience research is now uncovering. I will tell you which is which.
The Honest Short Answer
A meridian is a mapped line on the body. Along that line are specific points where, when stimulated by a needle, pressure, or heat, we reliably observe particular physiological effects — both locally and at sites distant from the needle. These maps were drawn over more than two thousand years of clinical observation in China and surrounding cultures, and they have been refined, debated, and revised continuously.
I am not asking you to take ancient theory on faith. I do not believe meridians are literal physical channels in the way an artery is a channel. If you opened up the human body looking for a “Lung meridian” the way you would look for the aorta, you would not find it as a discrete tube.
So what are they? The most useful analogy I have found is this: meridians are something like the wiring diagrams of an old building. The diagrams describe how signal moves through the structure — which switch controls which light, which circuit shares a breaker — even when the wires themselves run hidden behind plaster and you cannot point to them with your finger. The diagram is real and predictive even though the medium it describes is layered, distributed, and not always anatomically obvious.
The interesting question — the one I want every skeptical patient to sit with — is not “do meridians literally exist as channels?” The interesting question is: why do these specific points, in these specific patterns, reliably produce these specific effects? That is a question modern science has actually started to answer.
What Modern Science Has Found
Over the last twenty years, there has been a serious body of research looking at acupuncture points and meridian pathways using tools the ancient Chinese physicians did not have — MRI, electromyography, dissection of fascial planes, vagal nerve recording.
Three findings are worth knowing about.
First, fascia. Fascia is the connective-tissue web that wraps every muscle, organ, and vessel in the body. The work of Dr. Helene Langevin and her colleagues — including studies later supported by the U.S. National Institutes of Health — found that a striking proportion of classical acupoints sit at intersections of fascial cleavage planes. Some estimates put it around eighty percent. That means many of the points the ancient maps identified are at locations where the body’s connective-tissue architecture creates a physically distinct structure. The needle is not landing in random soft tissue.
Second, the autonomic nervous system. Several heavily studied points — Stomach 36 below the knee, Pericardium 6 on the inner forearm, Governing Vessel 20 at the crown of the head — have been shown to influence vagal tone, heart-rate variability, and parasympathetic activation. This is one mechanism by which acupuncture can produce the calming, regulatory effect that patients often describe — particularly relevant for the chronic pain conditions and stress-related complaints we see most often in clinic.
Third, brain imaging. Functional MRI studies, including work summarized by groups such as Cabioglu and others, have shown that needling true acupoints activates measurably different brain regions than needling nearby “sham” points. The pattern is not random.
Here is the honest framing: science has not validated meridians as literal channels. It has, however, validated that the points are real, anatomically meaningful, and reproducible in their effects. The “why” is still being worked out. The U.S. National Center for Complementary and Integrative Health (NCCIH) currently lists acupuncture as having credible evidence for several pain conditions, while being clear that the mechanism is not fully understood. That is a fair summary of where we actually are.
The 12 Primary Meridians (A Quick Map)
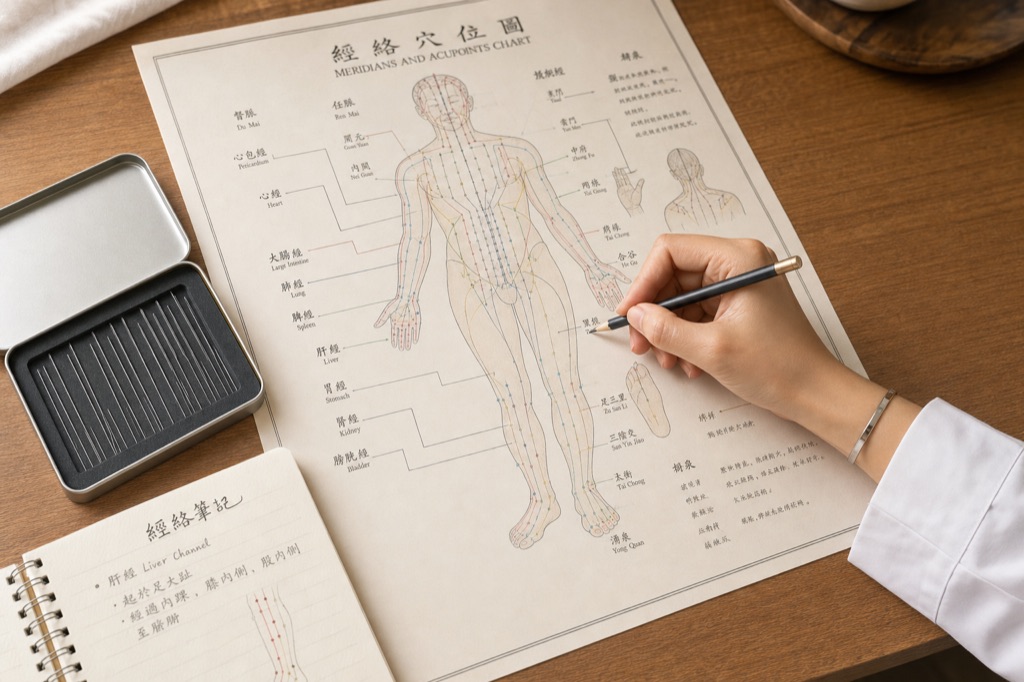
Classical TCM describes twelve primary meridians, each named after an internal organ:
Lung, Large Intestine, Stomach, Spleen, Heart, Small Intestine, Bladder, Kidney, Pericardium, Triple Burner, Gall Bladder, and Liver.
But the names are misleading to a Western reader. When TCM says “Lung meridian,” it does not only mean the anatomical lungs in the way your respirologist would mean. It refers to a broader functional system that classical Chinese medicine grouped together — in the case of the Lung, that includes respiratory function, the surface of the skin, the immune barrier, and, interestingly, the emotional process of grief.
This sounds strange at first. Why would the same “system” govern lungs and grief? But consider what modern psychoneuroimmunology has been finding: chronic grief and prolonged stress measurably suppress immune function and are associated with respiratory and skin conditions. The ancient framework grouped together what modern research is, by a different route, also discovering to be functionally connected.
So when I tell a patient I am working on her Liver meridian, I do not mean I am needling her liver organ. I mean I am addressing the functional pattern that classical theory associates with smooth circulation, emotional regulation (especially around frustration and stuck irritability), the sides of the body, the eyes, and certain types of tension headache. Whether or not you accept the classical explanation, the point selection along that pathway has been observed clinically for centuries to help with that cluster of symptoms.
The map is a tool. It guides where I put the needle. The reason it works is what the modern research is slowly uncovering.
A Real Clinical Example
A patient came to see me last month with chronic right-shoulder tension that had not responded to several months of physiotherapy. Her MRI was unremarkable — no torn rotator cuff, no impingement that would explain the persistent ache. She also mentioned, almost in passing, that she had been clenching her jaw at night, that her sleep had been broken for months, and that she felt easily irritated at work.
To a TCM-trained eye, that cluster — side-of-body tension, jaw clenching, disturbed sleep, irritability — points strongly toward a Liver-Gallbladder pattern. The Gallbladder meridian, in classical mapping, runs along the side of the head, down the side of the neck, across the top of the shoulder, and along the lateral aspect of the body. I needled along that pathway over three sessions, with attention to a few key points at the shoulder and the side of the neck.
Her shoulder released. The jaw clenching eased. She started sleeping through the night.
Why did it work? I can offer two frames, and both are useful.
The classical TCM frame: stress had created qi stagnation along the Liver-Gallbladder pathway, manifesting as tension where the meridian crosses the shoulder.
The modern hypothesis: needling along that fascial line produced a release pattern through the connected myofascial chain, while simultaneously shifting her autonomic nervous system out of a chronically activated sympathetic state. The shoulder was not just a local muscle problem; it was a downstream symptom of a system stuck in tension.
I do not need to choose between those frames. They describe the same outcome from different angles.
What Meridians Are NOT
I want to be just as clear about what meridians are not, because intellectual honesty cuts both ways.
Meridians are not magic. The word “energy” in TCM (qi) is a translation problem — it is closer to “functional capacity” or “regulatory signal” than to anything in a New Age sense. I am wary of any practitioner who talks about meridians in mystical terms.
Meridians are not a substitute for emergency medical care. If you are having chest pain, neurological symptoms, signs of stroke, or any acute medical event, go to the hospital. Acupuncture is not the right tool for those situations. It is also not a replacement for evidence-based treatment of serious illness — cancer, severe mental health crises, infections — though it may have a complementary role in supportive care.
Meridians are not validated by Western anatomy as discrete physical structures. As of today, no one has dissected a meridian the way you can dissect a nerve. Anyone who tells you otherwise is overstating the science.
What meridians are is a clinically useful map. The map predicts which points will help which patterns. That is what I work with.
How To Think About It as a Patient
Here is something interesting that the research has shown: you do not have to believe in TCM theory for acupuncture to produce measurable physiological effects. Studies looking at things like vagal tone and pain modulation show changes in patients who described themselves as skeptical going in. The physiology does not require your faith.
But understanding the framework is still useful, because it helps you communicate your symptoms in ways that I, as your acupuncturist, can act on.
A practical example. If you come in saying “my right shoulder hurts,” that is one piece of information. If you also mention that you grind your teeth, that you wake at three in the morning unable to fall back asleep, that your eyes feel tired, and that you have been more irritable than usual — now I have a pattern. In TCM thinking, those symptoms cluster together as a recognizable picture, and that picture guides which points along which meridian I will choose first.
So if there is one practical takeaway from this article, it is this: when you see an acupuncturist, do not just describe the loudest symptom. Mention the quieter ones too. Sleep, mood, digestion, body temperature, energy through the day. They are not unrelated; they are part of how we read your case.
A Note on Booking
If you are curious about whether acupuncture might help with what you are dealing with, the most useful first step is a sixty-minute initial assessment. That gives me time to take a proper history, look at the full pattern, and design a treatment plan that is specific to you rather than to a diagnosis label.
You can book at artemis.janeapp.com or call 604-242-2233. The clinic is at 5911 No. 3 Rd #130, Richmond BC, about two minutes’ walk from Brighouse SkyTrain station. We see patients in English, Mandarin, and Cantonese. Learn more about our Acupuncture & TCM service or read about specific applications including fertility acupuncture, chronic pain, and stress and burnout.
About the Author

Mandy Tam, R.Ac is the Founder and Lead Acupuncturist at Artemis Wellness Clinic in Richmond, BC. She is a Registered Acupuncturist with the College of Health and Care Professionals of British Columbia (formerly CTCMA), with more than ten years of clinical experience treating chronic pain, women’s health, sleep disorders, and stress-related conditions. Mandy practises in English, Mandarin, and Cantonese and serves patients throughout Richmond, Vancouver, Burnaby, and the broader Lower Mainland.
Reviewed by Mandy Tam, R.Ac · Published 2026-05-13
This article is educational only and does not constitute medical advice. Acupuncture is a complementary intervention; for serious medical conditions, please consult your family physician or appropriate medical specialist first. Individual responses to treatment vary.







