By Dave Tam, RMT · Director, Artemis Wellness Clinic Richmond BC
Reviewed by: Dave Tam, RMT · Date: [PENDING]
I’ve treated thousands of shoulders in the past decade. The same conversation happens at least once a week in my treatment room: “I stretch every day. I foam roll. I get massages. Why are my shoulders STILL tight by Wednesday?”
The honest answer is one most stretching guides won’t tell you: your shoulder tension probably isn’t a shoulder problem.
Here’s what I see in my clinic — and what actually works.
What “Tight Shoulders” Usually Means Anatomically
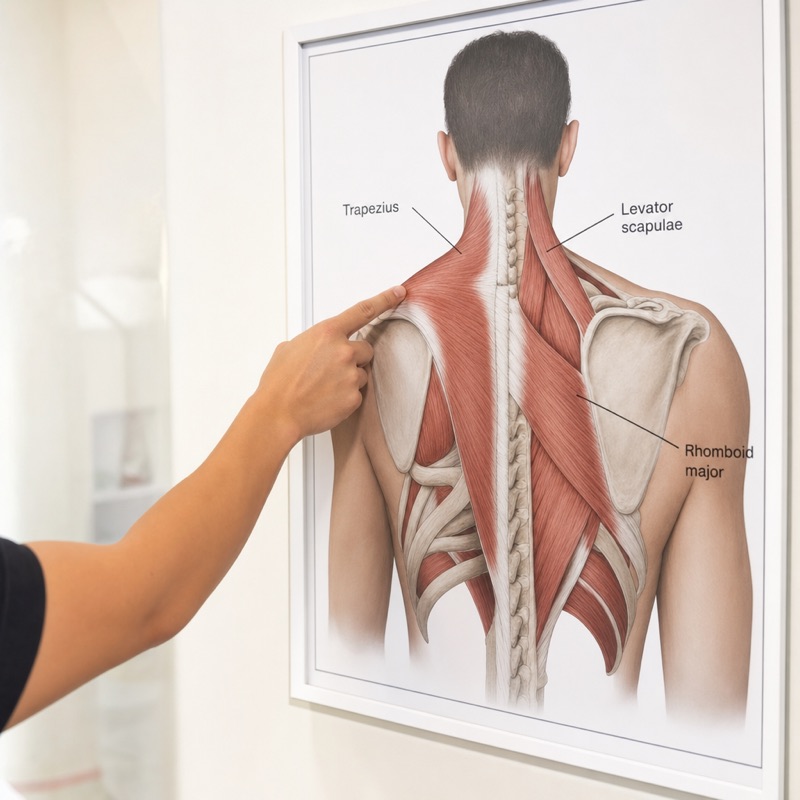
When someone walks into my room and says their shoulders are tight, they almost never mean their deltoids or rotator cuff. They’re pointing to that band of muscle that runs from the base of the skull down across the top of the shoulder and into the upper back. Anatomically, that’s a combination of three muscles working together: the upper trapezius, the levator scapulae, and sometimes the rhomboids underneath.
The upper trapezius fans out from the base of your skull and the upper neck vertebrae, attaching to the outer edge of your shoulder blade and collarbone. Its job is to elevate the shoulder blade, help rotate it upward when you raise your arm, and contribute to neck stabilization. The levator scapulae runs from the upper neck vertebrae down to the inner top corner of the shoulder blade — it lifts the shoulder blade and helps tilt the head. The rhomboids sit deeper, between the shoulder blades, pulling them toward the spine.
When patients describe a constant ache, knots, or that “wearing a backpack of bricks” feeling, these are the muscles I’m palpating. And here’s where the conventional advice goes wrong: these muscles are not tight because they are weak, lazy, or under-stretched. They are tight because they are working overtime — compensating for something else in the system that isn’t doing its job.
This is the single most important reframe I can offer. A muscle that won’t relax despite weeks of stretching isn’t a stretching problem. It’s a muscle that’s getting a constant signal to stay engaged. Stretching gives temporary relief because you’re forcibly lengthening fibres, but the moment you stand up and return to your day, the same nervous-system signal fires and the muscle clamps right back down. You haven’t changed the input — you’ve only briefly fought the output.
The 4 Real Root Causes I See in Clinic
In nearly every chronic shoulder-tension case I assess, the driver is one or a combination of the following four patterns. Each one explains why stretching fails and points toward what actually changes the pattern.
1. Forward head posture from screen work
When your head sits directly over your shoulders, the load on your upper traps is roughly the weight of your head — about 10 to 12 pounds. For every inch your head drifts forward of that neutral position, the load on the upper traps and posterior neck muscles increases by roughly another 10 pounds. Most desk workers I assess are sitting with their head 2 to 3 inches forward, which means their upper traps are holding 30 to 40 pounds, all day, against gravity.
Stretching the trap doesn’t reduce that load. The moment you sit back down at your monitor, the load returns. What works: raise your monitor so the top third of the screen is at eye level, practice chin tucks (gently drawing the chin straight back toward the throat) several times an hour, and strengthen the deep neck flexors so they can hold the head in a neutral position without recruiting the upper traps.
2. Inhibited or weak deep neck flexors and lower traps
This one is rarely mentioned in stretching content, and it’s the one I find most often. The deep neck flexors (the muscles at the front of the neck that should be holding your head up against gravity) and the lower trapezius (which should be pulling your shoulder blades down and stabilizing them) become inhibited in people who sit for long hours. When those postural stabilizers go offline, the upper traps and levator have to do all the postural work. They are not designed for that role. They become chronically over-recruited, and the brain interprets their constant low-grade contraction as “tightness.”
Stretching makes this worse, not better. When you stretch an over-recruited stabilizer without retraining the muscles that are supposed to be doing its job, the upper trap will simply re-engage harder afterward, because nothing else has come online to replace it. What works: lower trap activation drills (prone Y-raises are a good starting point) and deep neck flexor strengthening (chin tucks against a wall, slow and controlled). In my clinical experience, these two strengthening patterns produce more lasting relief than any amount of stretching.
3. Diaphragmatic breathing dysfunction (chest breathing)
This one surprises people. When you breathe with your chest instead of your diaphragm — meaning your shoulders rise on each inhale rather than your belly expanding — the scalenes (small neck muscles) and upper traps become accessory breathing muscles. They fire 14 to 18 times per minute, all day, every day. That’s roughly 20,000 extra contractions a day for muscles that were never designed for that load.
You can stretch and massage all you want; if you go right back to chest breathing, you are recruiting those muscles again within seconds. What works: diaphragmatic breathing retraining. Five minutes a day, lying on your back with one hand on your chest and one on your belly, practicing breathing so only the lower hand rises. Three weeks of consistent practice can dramatically reduce upper trap tone in patients I see — sometimes more than weeks of manual therapy alone.
4. Sustained low-grade stress and sympathetic nervous system overactivation
The shoulder girdle is one of the body’s primary “guard” zones. When the sympathetic nervous system is chronically activated — from work stress, sleep debt, financial worry, or just running too hard — the body holds a low-grade protective contraction across the upper back, jaw, and shoulders. This is evolutionary: protect the neck, protect the spine, prepare to fight or flee.
You can stretch a muscle that’s getting a constant neural signal to contract, but it’ll just contract again 30 seconds later because the signal hasn’t gone away. What works here is harder to package as a 5-minute fix: addressing nervous system regulation through better sleep, vagal tone work (slow exhales, cold exposure, humming), and sometimes counselling or therapy when stress has a clear source. I am not a mental health practitioner, but I can tell you that in my clinic, the patients who address their sleep and stress alongside the manual work are the ones whose shoulders actually stay loose.
A Real Clinical Example
Let me share a composite, anonymized example that captures what I see most weeks. Mr. K is a 38-year-old software developer in Richmond. He had been carrying upper-trap tension for 8 years. He had tried everything — daily stretching, yoga twice a week, an expensive foam roller, occasional massage every couple of months. Each time he would feel better for two or three days, then the tension would gradually creep back.
When he came in for an initial assessment, I spent the first 15 minutes not on his shoulders, but on the supporting system. I asked him to perform an isolated chin tuck — he could not activate his deep neck flexors without recruiting the upper trap simultaneously. I watched him breathe — almost entirely chest, shoulders rising visibly with each inhale. I asked about his desk setup — his monitor was about 4 inches lower than it should have been, putting him in mild forward head posture for 9 hours a day.
The treatment plan reflected the system, not the symptom. We did 3 RMT sessions over 3 weeks to release the over-recruited muscles and give his nervous system a reset. I gave him three home exercises (deep neck flexor activation, diaphragm reset, lower trap activation) and a single piece of equipment advice (a $25 monitor riser). I asked him to do the exercises twice a day for 6 weeks.
At our 6-week follow-up, his self-reported tension was reduced by about 80%, and more importantly, it wasn’t coming back the way it used to. The pattern had genuinely shifted. Why? Because we addressed the upstream drivers, not just the downstream symptom. The upper traps had finally been allowed to step out of the postural job they were never designed to do.
When Stretching DOES Work for Shoulders
I want to be fair to stretching. It is a useful tool — just not the right tool for every problem. Stretching works well for: acute post-exercise tightness that resolves in a day or two; mild generalized tension after a particularly stressful day where your nervous system just needs a wind-down ritual; and as part of a movement warm-up before exercise. If your shoulders feel cranky after a long hike or a tough workout, by all means stretch. That is exactly what stretching is for.
What stretching is honestly not for is the chronic, weeks-or-years pattern of constant tension that returns no matter how much you stretch. That pattern is signalling something deeper, and the body is asking you to look at the system, not just lengthen the fibres.
A Better 5-Minute Daily Practice
Here is what I actually give my patients as a starting home program. Five minutes, no equipment, done in this order:
- Diaphragm reset (1 minute). Lie on your back, knees bent, one hand on your chest and one on your belly. Breathe slowly so only the hand on your belly rises and falls. This resets your default breathing pattern away from chest breathing.
- Deep neck flexor activation (1 minute). Stand against a wall with the back of your head touching it. Gently draw your chin straight back toward your throat (without tilting your head down) so the back of your skull presses lightly into the wall. Hold for 3 seconds, release. Ten slow repetitions.
- Lower trap activation (1 minute). Lie face down on a bed or the floor with your arms extended overhead in a Y shape, thumbs pointing up. Lift your arms slightly off the surface, focusing on squeezing the muscles between and below your shoulder blades. Ten slow repetitions.
- Pec doorway stretch (1 minute). Only after the three activation drills above. Stand in a doorway, place your forearm on the door frame at shoulder height, and step gently forward until you feel a stretch across the front of your chest. Hold 30 seconds per side. Tight pecs pull the shoulders forward, so we stretch them so the back muscles can do their job.
- Shoulder roll-down (1 minute). Not the foam roll. Stand or sit, slowly raise both shoulders up toward your ears, hold the contraction for 3 seconds, then fully release and let them drop. Five repetitions. This trains your nervous system to recognize what a relaxed baseline actually feels like — which most chronic-tension patients have honestly forgotten.
Note the order: we restore breathing, activate the underused stabilizers, then stretch the muscles that are pulling things forward, then teach the nervous system to find baseline. This sequence matters more than any one of the steps alone.
When To Book Professional Care
Home work is the right starting point for most people. But there are cases where you need a hands-on assessment. Book an appointment if: your tension has lasted 6 months or longer despite consistent home work; you are getting headaches or jaw pain alongside the shoulder tension; the home program above has not moved the needle in 3 to 4 weeks of consistent practice; or you are noticing numbness or tingling radiating into your arms or hands. That last one is a red flag — it can indicate cervical nerve involvement and warrants a proper assessment, ideally in coordination with your physician.
Closing
If your shoulder tension isn’t responding to home work, an initial RMT assessment can identify which of the four root causes is driving your pattern. That clarity alone tends to change how patients approach their bodies. Book at artemis.janeapp.com or call 604-242-2233. We’re at 5911 No. 3 Rd #130, Richmond BC, steps from Brighouse SkyTrain. See also: our 5 daily office stretches done right, Richmond RMT techniques explained, and our hybrid worker neck and back guide.
About the Author

Dave Tam, RMT is a Registered Massage Therapist regulated by the College of Massage Therapists of British Columbia (CMTBC). He is the Director of Artemis Wellness Clinic in Richmond, BC, where he leads the RMT team and specializes in chronic tension patterns, post-injury recovery, and athletic performance care. Dave co-founded Artemis with his sister Mandy Tam in 2025.
Reviewed by Dave Tam, RMT · Published 2026-05-13
This article is educational only and does not constitute medical advice. The home exercises described are general guidance — for an individualized plan, see a regulated practitioner. If you experience numbness, tingling, weakness, or sudden severe pain, consult a physician.