BC ice hockey season runs from September through March, with the heaviest game density between October and February. For the thousands of recreational, masters, beer-league, and pickup players in Richmond who skate at local arenas across the Lower Mainland, the season is long, the ice is cold, and the bodies are — for most of us — no longer twenty-five. Artemis Wellness Clinic at 5911 No. 3 Rd #130, Richmond BC V6X 0K9 — steps from Brighouse SkyTrain — supports hockey players across the full season with five coordinated disciplines under one roof: RMT, acupuncture, physiotherapy, chiropractic, and kinesiology. Book online at artemis.janeapp.com or call 604-242-2233.
This guide covers pre-season conditioning (August–September), mid-season maintenance (October–February), the most common hockey injuries we see in our in-clinic rehabilitation space, and how to tell whether a flare-up is something you can train through or something that needs a same-week assessment.
Why Hockey Season Demands Its Own Recovery Rhythm
Hockey is not just “another team sport.” Four sport-specific factors change what your body needs across a six-month season:
Arena temperature shock. You arrive in a warm car, walk through a refrigerated arena, sit on a cold bench, then sprint at 90% effort in 45-second bursts. Cold muscles do not lengthen well, and the warm-cold-warm-cold cycle through a game is unique to ice sports. Groin and hip flexor strains in the first ten minutes of a game almost always trace back to inadequate warm-up against the cold environment.
Skating biomechanics. A skating stride loads the hip in a way no other sport does — deep hip flexion, powerful hip extension, and forced external rotation, all on a narrow blade. Adductor (groin), iliopsoas (hip flexor), and gluteus medius are the muscles that absorb this load. Over a season, asymmetries between left and right strides accumulate into the chronic groin tightness most masters players just call “hockey hips.”
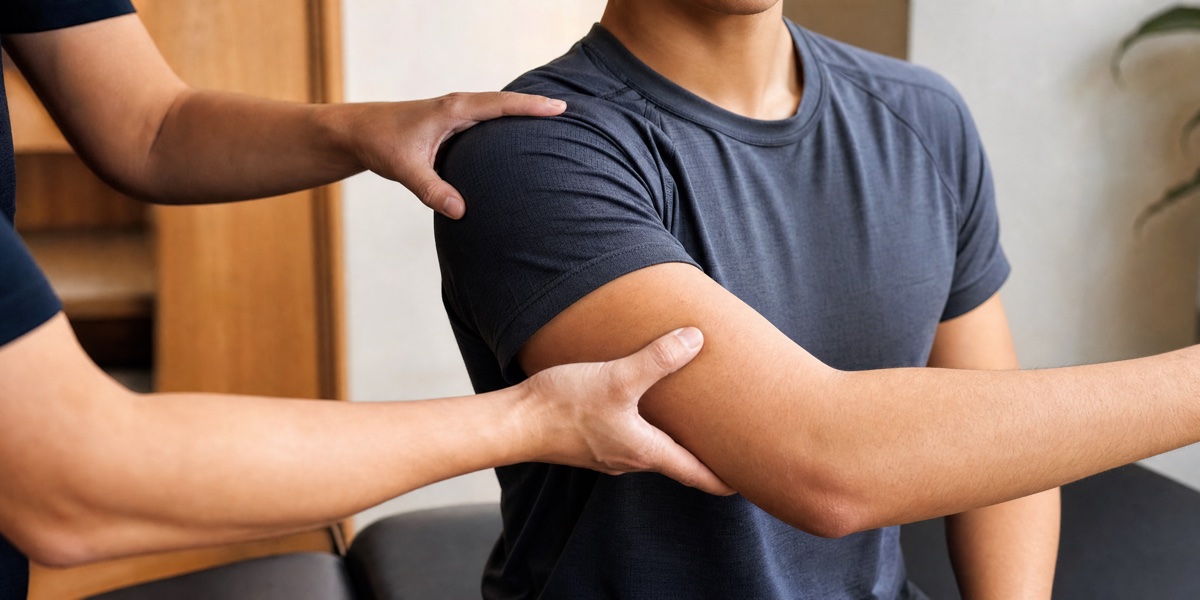
Body contact, even in non-contact leagues. Adult rec leagues are nominally non-contact, but boards, falls, stick collisions, and shoulder bumps are part of the game. The acromioclavicular (AC) joint in the shoulder takes the brunt of most falls onto the ice. Lower back pain from being checked or bracing against the boards is a weekly occurrence in our clinic from October onward.
The “game-then-immediate-beer” pattern. This is the most common recovery mistake we see. A one-hour late-evening game, a hot dressing room, then sitting in a pub at 10:30 PM with cold beer and no stretching, no hydration, no flush of the legs. Inflammation never gets cleared, sleep is poor because of late food and alcohol, and you wake up Wednesday for your next skate already behind. The pattern compounds across a season.
Each of these patterns has a counter-strategy. The right care at the right point in the season is the difference between finishing March feeling strong and limping into spring with a chronic groin strain that follows you into summer.
Pre-Season Conditioning (August–September)
If you only do one block of intentional preparation, do it in the six to eight weeks before your league starts. Three priorities:
Off-ice strength, especially posterior chain. Glutes, hamstrings, and lower back are your insurance policy against the most common in-season injuries. A short twice-weekly routine — hip thrusts, single-leg Romanian deadlifts, side planks — covers the foundation. A single kinesiology consult to build a 4-week pre-season program is high-leverage; see our from ICBC discharge to performance guide for the rebuilding philosophy we use, which applies just as cleanly to pre-season prep as to post-injury return.
Hip mobility. Hockey’s deepest demand is hip range of motion under load. Daily 10-minute mobility work — 90/90 rotations, deep squat holds, hip flexor stretches — through August builds a buffer that the season will eat into. Combine with a 60-minute pre-season RMT session focused on adductors, hip flexors, and quadratus lumborum to release any summer-accumulated tightness.
Skating-specific conditioning. Cardiovascular conditioning that matches hockey’s interval profile — short, intense, repeated efforts — is more useful than steady-state running. Stationary bike intervals (30 seconds hard, 30 seconds easy, repeated 12 times) come closer to a hockey shift than a 5K jog does.
What we do NOT recommend in pre-season: deep tissue massage three days before your first league game, brand-new training programs in the final week, or skipping the off-ice work because “I’ll get into shape during the season.” That last one is the leading cause of Week 2 groin strains in our clinic every fall.
Mid-Season Maintenance (October–February)
Once games are weekly, the goal shifts from building to maintaining. The maintenance pattern that works for most rec and masters players:
A 60-minute massage every two weeks. Focus rotates between adductors/hip flexors (the highest-demand area), quadratus lumborum and gluteus medius (low back and hip stabilizers), and upper-body work for shoulders and forearms (especially for goalies and defencemen). See our registered massage therapy in Richmond guide for what to expect from your first session and how RMT integrates with our other services.
Acupuncture for sleep. Late-evening games and the post-game adrenaline spike disrupt sleep for many players. Acupuncture protocols for nervous system downregulation help measurably with the Tuesday-night-game-Wednesday-tired pattern. Many of our masters-league patients book monthly acupuncture sessions specifically for sleep, with secondary benefit for chronic muscle tension.
One mid-season kinesiology check-in around mid-December. By this point in the season, most players have at least one minor asymmetry they have been ignoring. A 45-minute movement screen catches things before they become February problems. This applies especially to players over 35 — see our weekend warrior and masters athlete guide for the broader framework around recreational athletes who train hard around full-time work.
Common Hockey Injuries We Treat
Five injuries account for most of our hockey caseload. We treat them within our broader team sports injury rehab framework, which integrates physiotherapy, RMT, acupuncture, and kinesiology depending on the injury phase.
Groin (adductor) strain. The single most common hockey injury. Sharp pain in the inner thigh during a stride, often after an inadequate warm-up. Mild strains respond to two to three weeks of modified training plus combined physiotherapy and RMT. Moderate strains need a structured 4 to 6 week return-to-skate plan.
Hip flexor (iliopsoas) strain. Pain at the front of the hip, especially when lifting the knee or accelerating. Often presents alongside lower back pain because the iliopsoas attaches to the lumbar spine. Treatment combines manual release, targeted strengthening, and sometimes acupuncture for muscular guarding.
Lower back pain. Common in defencemen who absorb checks against the boards and in players with weak posterior chain. Most non-traumatic lower back pain in hockey players responds well to combined physiotherapy and RMT — see our dedicated lower back pain treatment in Richmond guide for the symptom-side detail and treatment options.
AC joint shoulder injury. From falls onto the ice or shoulder-to-shoulder collisions. Mild AC joint sprains (Grade 1) usually settle with relative rest plus targeted physiotherapy over 2 to 4 weeks. Moderate to severe AC injuries need imaging and may require referral to a sports medicine physician — we will tell you honestly which category you are in.
Concussion. A specific note here: Artemis does not provide specialized concussion treatment. We do not run baseline ImPACT testing, we do not have a concussion-trained physiotherapist on staff, and we do not manage return-to-play decisions for concussion. If you have suffered a head impact and have any symptoms — headache, nausea, dizziness, light or sound sensitivity, sleep disruption, fogginess — see your family doctor or a concussion specialist clinic. We are happy to coordinate supportive care (RMT for neck stiffness, acupuncture for sleep) once a concussion specialist has cleared you for that, but the primary management belongs with someone trained in it. This is the kind of honest scope-of-practice line we draw across all our service guides.
Acute Injury vs Chronic Pattern: When to Come In
Two different timelines depending on which side of the line you are on.
Acute injuries — sharp pain that happened on a specific shift, or a fall you remember — get assessed within 48 to 72 hours. Earlier intervention almost always shortens the recovery curve. Do not “wait and see” if it is still painful by Wednesday after a Sunday game; book an assessment.
Chronic patterns — the groin tightness you have had for a month, the lower back stiffness that comes and goes, the shoulder that clicks but does not really hurt — get treated on the maintenance schedule. Add a 60-minute physiotherapy assessment to your next regular massage booking; we can usually identify whether it needs active rehab or just consistent soft-tissue work.
The pattern to avoid: ignoring a chronic mild injury for two months, then having it become acute when you fall on it during a game. Most of our February emergency bookings could have been a December maintenance booking.
Coordination With Kinesiology for Return-to-Skate After Injury
For any injury that takes you off the ice for more than two weeks, the return-to-skate plan matters as much as the injury treatment itself. Our kinesiologists work with players returning from groin strains, lower back injuries, and shoulder injuries to design a graduated plan that bridges from clinic exercises to power skating to scrimmage to full game play.
A typical return-to-skate sequence: pain-free off-ice strength work → solo skating drills at low intensity → solo skating with stride power → small-area scrimmage → full game pace. Each step needs to be tolerated for two to three sessions before progressing. Skipping steps is the most common reason for re-injury within the first month back. The same kinesiology framework we describe in our from ICBC discharge to performance guide applies cleanly here — bridging from finished medical recovery back to full sport capacity is the same problem regardless of how the injury happened.
Frequently Asked Questions
How often should I get a massage during hockey season?
For most rec and masters players, every two weeks is the maintenance sweet spot. Players over 45 or those playing twice a week often benefit from weekly sessions during peak season (November–February). Pre-season and post-season can drop to monthly.
Do you treat youth hockey players?
Our primary audience for this guide is adult rec and masters players, but we do see teenage hockey players for specific injuries (especially groin and hip flexor strains). For younger children, we generally recommend coordinating with a paediatric-focused practitioner and the team trainer.
Can acupuncture help with hockey-related sleep problems?
Yes — well-evidenced acupuncture protocols for nervous system downregulation help with the late-evening-game sleep disruption that many adult players experience. Book a 60-minute session weekly for 3 to 4 weeks initially, then maintain monthly.
My groin has been tight for two months but it doesn’t really hurt. Should I come in?
Yes. Chronic mild adductor tightness is the precursor to most acute groin strains in mid-season. A 60-minute combined RMT and brief physiotherapy assessment is the right starting point.
Do you do concussion treatment?
No. We do not provide specialized concussion management or return-to-play clearance. If you have head-impact symptoms, see a family doctor or a concussion-specialist clinic first. We can support recovery (neck and upper-back work, sleep-focused acupuncture) once a concussion specialist has cleared that.
Do you direct bill for hockey injuries?
Yes for extended health insurance (Pacific Blue Cross, Sun Life, Manulife, Canada Life, Green Shield) under standard physiotherapy / RMT / acupuncture / chiropractic line items. ICBC and WorkSafeBC apply only if your hockey injury is part of a separate covered claim.
What about goalies — different recovery needs?
Yes. Goalies load the hips even more aggressively (deep butterfly position) and the shoulders far less than skaters. Goalie-focused maintenance leans heavily on hip mobility, adductor work, and lower-back care. We adjust the session focus accordingly.
I play in a Sunday-evening league. Can I get a Monday morning recovery massage?
Yes — we have weekday-morning availability across most disciplines. Check live availability on Jane App for same-week or next-day slots.
Recover and Stay Skating at Artemis
Whether you are prepping for a September league start, mid-season and trying to nurse a chronic groin through to playoffs, or recovering from an acute injury and planning your return to ice, the right care at the right point in the season is the difference between finishing March strong and starting next September from scratch. Artemis Wellness Clinic, 5911 No. 3 Rd #130, Richmond, BC V6X 0K9 — steps from Brighouse SkyTrain. Five regulated disciplines coordinated under one roof: RMT, acupuncture, physiotherapy, chiropractic, kinesiology. Book online at artemis.janeapp.com or call 604-242-2233. Direct billing for ICBC, WorkSafeBC, and most major extended health plans. Weekday-evening and Saturday daytime availability — important when you have a game tomorrow night.